
Mental health treatment has evolved significantly over the past decade. While therapy and medication remain foundational tools, advances in neuroscience have created additional options for individuals who need something different.
One of the most established and research-supported of these options is Transcranial Magnetic Stimulation (TMS).
At
Blue Umbrella Psychiatry, we provide TMS therapy for adults with treatment-resistant depression, individuals with OCD, and adolescents with depression — and in many cases, treatment may be covered by insurance.
What Is TMS?
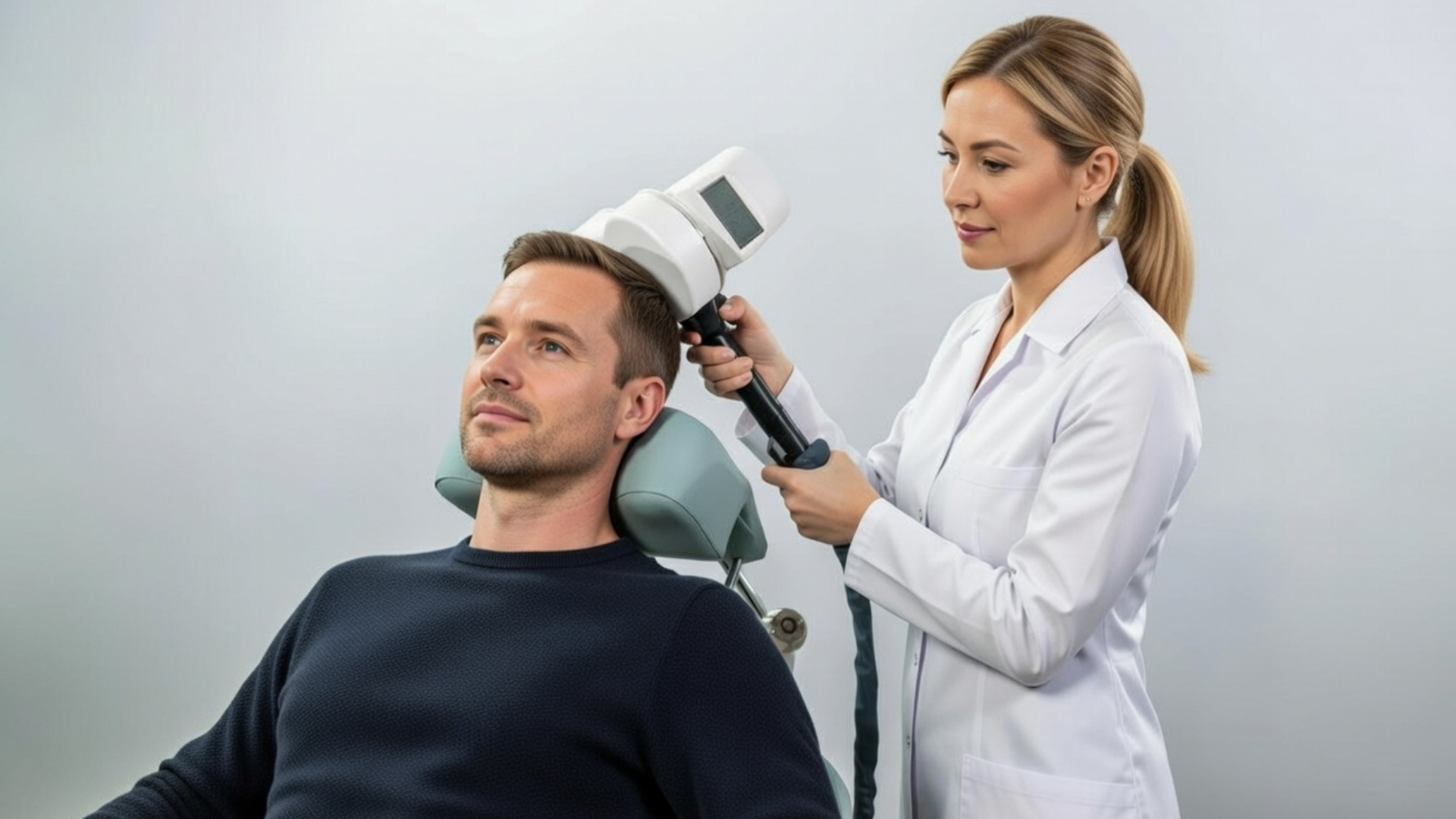
Transcranial Magnetic Stimulation is a non-invasive, FDA-cleared treatment that uses targeted magnetic pulses to stimulate specific regions of the brain involved in mood regulation and cognitive control.
Rather than affecting the entire body like medication, TMS works locally — activating or modulating neural circuits directly connected to depressive and obsessive-compulsive symptoms.
Treatment is delivered in-office. Patients remain awake, seated comfortably, and able to resume normal activities immediately after each session.
There is:
- No anesthesia
- No sedation
- No systemic side effects associated with medication
- No recovery time

TMS for Treatment-Resistant Depression (TRD)
For individuals who have tried antidepressants without adequate relief, TMS offers a different approach.
In depression, certain brain regions responsible for mood regulation may show reduced activity. TMS uses repetitive magnetic stimulation to increase activity in these underactive areas, supporting improved communication within mood networks.
A typical course of treatment involves sessions five days per week over several weeks, with each appointment lasting approximately 20–40 minutes depending on the protocol.
Improvement is often gradual and cumulative as neural pathways strengthen over time.
TMS for OCD
TMS is also FDA-cleared for Obsessive-Compulsive Disorder.
OCD involves hyperactive circuits in areas of the brain responsible for intrusive thoughts and repetitive behaviors. Specialized TMS protocols are designed to help regulate this overactivity, reducing the intensity and frequency of obsessive-compulsive symptoms.
For patients who have not responded fully to medication or exposure-based therapy, TMS can serve as an additional evidence-based option.
TMS for Adolescents

TMS has expanded to include FDA clearance for adolescents with depression, offering a structured and non-medication-based treatment option for teens struggling with moderate to severe symptoms.
For families concerned about medication side effects or limited response to traditional treatment, TMS may provide an alternative path that is closely monitored and clinically guided.
As always, candidacy is determined through comprehensive psychiatric evaluation.
Insurance Coverage
Unlike some emerging treatments, TMS is frequently covered by insurance when medical necessity criteria are met.
Coverage commonly applies for:
- Treatment-resistant depression
- CD
- Adolescent depression (depending on plan requirements)
Our team assists with benefits verification and prior authorization to determine eligibility and guide patients through the approval process.
What Makes TMS Different?
TMS does not introduce new medication into the body.
It does not require sedation.
It does not involve memory disruption.
Instead, it works by stimulating specific neural pathways associated with mood and compulsive behavior — helping the brain reestablish healthier patterns of activity.
For some individuals, this precision-based approach makes a meaningful difference when other treatments have plateaued.
What Makes TMS Different?
TMS does not introduce new medication into the body.
It does not require sedation.
It does not involve memory disruption.
Instead, it works by stimulating specific neural pathways associated with mood and compulsive behavior — helping the brain reestablish healthier patterns of activity.
For some individuals, this precision-based approach makes a meaningful difference when other treatments have plateaued.













