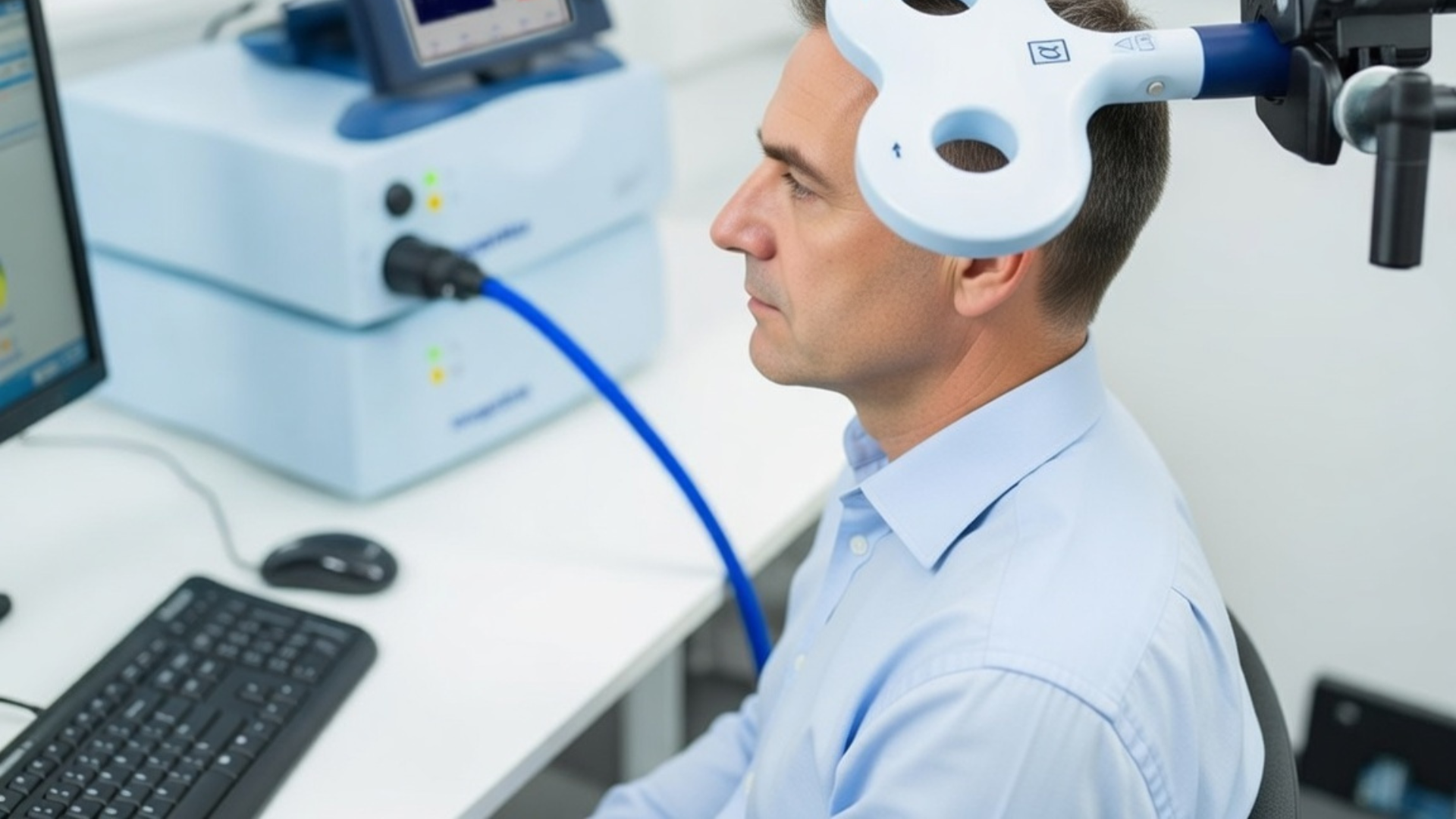
IT's not you, it's the brain
TMS, or transcranial magnetic stimulation, is an FDA-approved treatment that uses magnetic pulses to stimulate the root cause of depression in the brain. It's safe, highly-effective, and covered by insurance. Depression is caused by a lack of sufficient activity in the left dorsolateral prefrontal cortex, essentially the front left part of your brain. When the area is working properly, the entire brain lights up, resulting in an improved mood, working memory and selective attention.
About 75% of patients who complete a full course of TMS show a clinically meaningful response and
about 50% experience a full remission, meaning their symptoms go away completely. Sessions are about 20 minutes and you can drive to and from your appointments. The full course covered by insurance usually takes about 6-8 weeks to complete.
But how do you know if it’s right for you?
All major payers cover TMS treatment for Depression. If you've tried multiple antidepressants and therapy, there's a good chance your insurance covers it. We know - sometimes therapy or medication alone is not enough. When depression shows no improvement after trying these methods, it’s considered Treatment Resistant Depression. Treatment-Resistant Depression occurs as high as
60%
of all people with depression. Treatment-Resistant Depression is used to define a lack of success after at least two medication trials (usually different medications with various dosages) and/or at least 12 sessions of evidence-based psychotherapy.
Even when receiving high-quality care, 50% of people with depression will experience
NO
symptom reduction. In addition, people with TRD are twice as likely to be hospitalized. It is certainly not something to be taken lightly and additional treatment (such as TMS) should be considered promptly.
When this occurs, it is so easy to become discouraged or believe that you’re a hopeless cause.
This simply is not true!
Clients and therapists alike may be disheartened at the lack of progress; however, it’s not necessarily the therapist or client. The client just might need extra care in addition to therapy.
As mentioned above, TMS has remarkable success rates and is entirely safe and painless. TMS therapy is FDA approved with no long-term side effects. It is well-tolerated and does not require any kind of sedation or anesthesia. It’s also safe for any patients that are pregnant or breastfeeding.
Blue Umbrella Psychiatry is here and ready to come alongside you on your journey to find healing and happiness!
Reviewed by Dr. Eric Robbins, MD
References
Berman, R. M., Narasimhan, M., & Charney, D. S. (1997). Treatment‐refractory depression: Definitions and characteristics.
Depression and Anxiety,
5(4), 154–164.
Gaynes, B. N., Lux, L., Gartlehner, G., Asher, G., Forman‐Hoffman, V., Green, J., Boland, E., Weber, R. P., Randolph, C., & Bann, C. (2020). Defining treatment‐resistant depression. Depression and Anxiety, 37(2), 134–145.